Joint disease is a disabling and common complication of severe (and, to a lesser extent, moderate) hemophilia A. For people living with hemophilia A, joint damage refers to the damage caused by the repeated bleeding in and around the joint cavity. Permanent damage can be caused by one serious joint bleed (hemarthrosis).
Prophylactic therapy is effective in preventing recurrent bleeding episodes into joints and muscles. However, despite this success, bleeding in these areas is still a problem and a major manifestation of the disease.
Bleeding most commonly occurs in the knees, elbows, and ankles, and is often evident from early childhood.
The damage to the joint of a person with hemophilia A is similar to the damage to the joint of a person with arthritis. It occurs in two places in the joint.
Healthy Joint
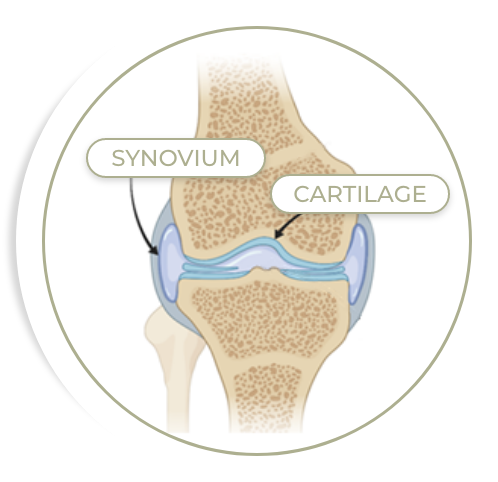
Damaged Joint
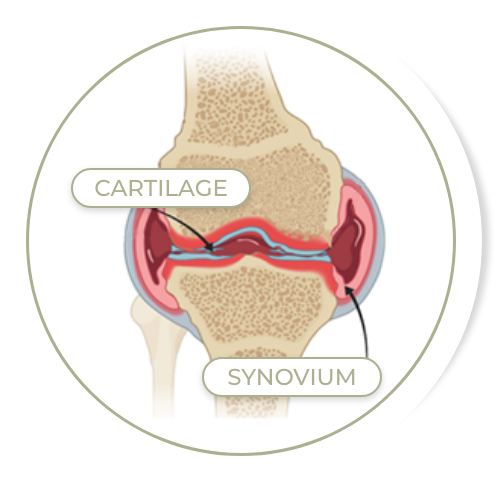
Thin lining on the inside of the joint, with three functions:
- lubricate joint
- feed cartilage
- remove fluid and debris from joint
The synovium has many blood vessels, which is one of the reasons why joint bleeding is so common in hemophilia A.
The synovium absorbs the blood in an attempt to remove it, and the iron in the blood accumulates which is thought to cause the synovial lining to thicken. The thicker the synovium is, the more blood vessels it contains, making bleeding more likely.
The type of cartilage that impacts those with hemophilia A is the one that forms a smooth hard cap on the ends of the bones that form the joint, allowing the bones to glide over each other without friction. This cartilage gets eaten away by enzymes from the swollen synovium.
If joint bleeding is not treated adequately, it tends to recur, resulting in a vicious cycle that must be broken to prevent the development of chronic inflammation of the connective tissue that lines the inside of the joint capsula (aka synovitis) and degenerative arthritis.
Joint damage can be prevented
Optimal management requires early prevention and treatment of joint bleeds before the onset of degenerative disease.
Prophylactic factor replacement therapy from an early age is the best method for preventing and/or reducing the risk of joint bleeds and joint disease (arthropathy).
You can also limit the permanent effects of a bleed with:
- Rest (to allow the bleeding to stop)
- Elevation of the limb (to lower the blood pressure and allow the blood to drain away)
- Electrical stimulation to improve strength
Physiotherapy is also important to: help preserve movement and function of the joints; reduce swelling and pain; maintain muscle strength; and prevent injury.
Preventive physiotherapy can be used to help strengthen the muscles surrounding the joints, and to improve mobility, flexibility, and balance.

