Nosebleeds in children with bleeding disorders
Nosebleeds (also known as epistaxis) are a common occurrence in children, especially those with an underlying bleeding disorder such as hemophilia. They can occur at any time but tend to cause more disruption when they occur at school, during activities with friends or when away from home. Nosebleeds can cause panic and anxiety but understanding more about them can help ease these feelings.
Basic anatomy of the nasal cavity
The nasal cavity extends from the nostrils to the back of the throat.
- The area is lined with a very thin layer of tissue called a mucous membrane.
- Beneath the mucous membrane is a large collection of tiny, very fragile blood vessels.
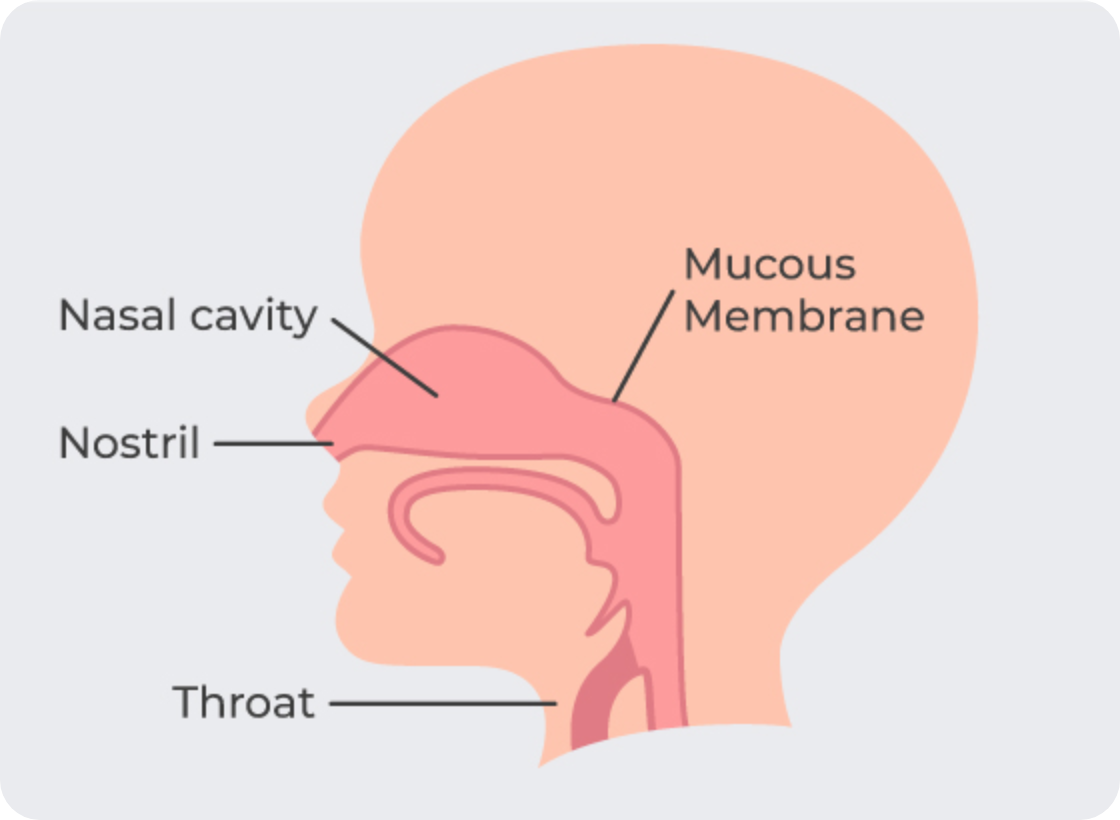
What causes a nosebleed?
Any time one of these blood vessels is damaged, a nosebleed may occur. If the bleeding vessel is towards the back of the nasal cavity then blood can trickle down the back of the throat into the stomach, rather than out of the nares (nostrils).
Common contributing factors
There are a number of factors that can make nosebleeds more likely to occur in children:
- Nose picking that causes damage to the mucous membrane lining the nostrils
- Trauma, which can include a direct injury to the nose, but may also include forceful sneezing or blowing
- Dry air, lack of moisture, often worse in the winter months or allergy season
- Natural structure of the nose and nasal cavity, such as a deviated septum or thin mucous membranes
-
Genetic predisposing factors such as a bleeding disorder
- Children with bleeding disorders are prone to more serious nosebleeds, especially when they have very low levels of the affected protein.
What to do if your child has a nosebleed
When a child has a nosebleed, it is really important to remain calm. The bleeding is less likely to stop if the child is panicked or crying.

- Have your child sit down and tilt their head slightly forward. Avoid tilting the head back, as blood can trickle down the throat into the stomach, causing vomiting.

- Have them gently blow their nose to clear the nasal passage of any fresh blood or soft clots.

- Firmly pinch the nose just beneath the cartilage, where the nose is soft.
- Don’t ease up on the pinching for at least 10-15 minutes.
- After 15 minutes, you can check to see if the bleeding has stopped. Ideally a clot will form so it is important to avoid blowing the nose immediately after the bleeding has stopped. Dislodging that clot will likely cause the vessel to bleed again. If the bleeding hasn’t stopped, hold pressure for 5 more minutes.
Tips
- Keep nails short to avoid accidentally scratching the inside of the nose, and avoid picking the nose.
- It is important NOT to stick tissue up the nose.
- Tissue will stick to the clot, therefore removing the tissue will take the clot with it and cause re-bleeding.
- If your child experiences nosebleeds often, consider having a “nosebleed kit” handy.
- It could include clean washcloths (the darker the better), disposable gloves, and cleaning wipes.
- Inform your child’s school/daycare that they are prone to nosebleeds.
- Provide them with a clear set of instructions on what to do should it happen and tell them that you would like to be notified.
- Your hemophilia treatment centre may have some resources that you can give to the school/daycare.
- Consider keeping a journal to record nosebleeds. This is likely information you will be asked for if you seek medical care. Important things to note are:
- Did the nosebleed involve one or both nostrils?
- How long did the nosebleed last?
- Were there clots?
- Are there any factors you think may have contributed? Are they occurring in clusters, or is there any pattern you notice?
- Your child may need to see an ear, nose and throat (ENT) specialist. This will require a referral from your hematologist or family physician.
Pharmacologic interventions (always check with your HTC)
- Factor replacement products
- Antifibrinolytic agents (a medicine taken by mouth to prevent the breakdown of clots)
- Lubricating creams or ointments to keep the mucous membranes of the nostrils moist
Non-pharmacologic interventions
- Increase moisture in dry months: place a humidifier in the child’s bedroom.
- Place lubricating gel (i.e., Vaseline) inside the nostrils.
- This will also help to moisturize air entering the nasal cavity.
- Use saline sprays to help keep the nostrils moist.
- Use a flexible ice pack or something similar—and protect skin from ice burn.
- Nasal cautery, a procedure done by an ENT Specialist
- Chemical seals the mucous membrane and stops the bleeding.
While most nosebleeds are minor, there are times when you may need to seek further medical attention:
- Nosebleed lasting longer than 20 minutes
- Bleeding is rapid or blood loss is large (more than a cup)
- Difficulty breathing
- Vomiting due to swallowing a large amount of blood
- Signs of anemia (feeling weak or faint, tired, cold, short of breath, pale skin)
- Recurrent (cluster) nosebleeds
- Often occur when the same vessel doesn’t heal between bleeds
- May occur from the same nostril 4 days per week or more
- Any loss of consciousness
A nosebleed can look scary, but is usually not a serious problem. The more informed and prepared you are, the better. If you have any more questions, please talk to your doctor.

